Cost-Effective Operations and Maintenance for COVID-19
By ED LIGHT, CIH, and PAUL TSENG, P.E., LEED Fellow
COVID-19 is most often transmitted directly from an infected individual to another in close proximity, and neither HVAC operation nor sanitizing can prevent this. However, the risks of transmission can be mitigated using methods well known to be effective with other similarly transmitted viruses.
While costly upgrades to HVAC and deep cleaning are being strongly advocated to address the pandemic, available information suggests that relatively minor HVAC adjustments and cleaning enhancements may be sufficient to minimize COVID-19 spread to help building owners and facility managers to reopen their buildings safely without budget busting measures.
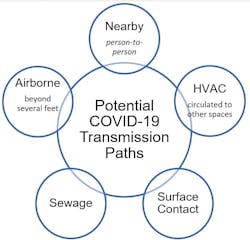
Understanding how COVID-19 is being spread in buildings is critical to identifying the measures which are most likely to reduce health risk. Available information on the different types of COVID-19 transmission suggests:
- Nearby Exposure –The majority of COVID-19 cases are associated with nearby exposure defined as within several feet of an infected individual;
- Airborne Transmission – Exposure beyond several feet appears to be relatively infrequent. Although SARS-CoV-2 (the virus causing COVID-19) is found in the air at considerable distances from an infected occupant, studies associated COVID-19 spread with poor ventilation (negligible exchange with outdoor air);
- HVAC Transmission – Virus circulated to another space via HVAC systems has not been documented;
- Surface Transmission – Transmission by contact with contaminated surfaces has not been documented but is assumed based on experience with similar viruses;
- Sewage Transmission – The exposure to virus-contaminated droplets from sewage, including toilet flushing and sewer gas has not been studied to see if it is responsible for spreading COVID-19.
Current Evidence Related to The Role of HVAC in COVID-19
Most air sampling for SARS-CoV-2 has only measured the total amount of virus in air (based on analysis for RNA). However, most of these studies measured only total virus, a parameter which may or may not include active virus (the type that causes infection). One field survey has detected infectious virus in indoor air, and that was where COVID patients were being treated in a hospital. No research has found SARS-CoV-2 discharged from re-circulating HVAC systems. Sites have recently been documented where samples of filters and exhaust duct surfaces tested positive for total virus but were negative for infectious virus.
Several outbreak investigation studies have associated COVID-19 with airborne transmission. A common factor among these studied site conditions was poor ventilation, in some cases, air flow patterns potentially concentrated virus in the breathing zone. One outbreak investigation found no COVID-19 cases in rooms with good ventilation despite the fact that air was being recirculated from rooms housing infected occupants. New cases in this study only occurred where the cabin-mate was already infected (nearby transmission). One study has reported occupants infected by the virus moving between floors through a transfer duct (no fan). No epidemiological studies have shown a benefit from enhanced ventilating or filtration. Evaluation of global COVID-19 patterns concluded that they are consistent with nearby transmission being dominant and airborne transmission only occurring occasionally.
Research to date has been insufficient to draw firm conclusions on HVAC’s actual contribution to COVID-19 spread. Available information suggests that HVAC can be a contributing factor in some cases but does not have a significant impact overall.
Modifying HVAC to Reduce COVID-19 Spread
Ventilation
HVAC can reduce exposure by diluting or removing the virus but can also increase infection risk by concentrating virus in the breathing zone (problematic air flow patterns). Many options are available for increasing mechanical ventilation. Because many facilities are not able to keep up with maintenance, systems are often not providing the intended ventilation (i.e., dampers stay closed, controls not set correctly). Resolving deferred maintenance deficiencies, especially in areas in with poor ventilation, is the single most cost-effective way to reduce virus exposure while also improving occupant comfort and indoor air quality
Another cost-effective way to address HVAC deficiencies may be to simply adjust occupancy. Examples for doing this include delaying or limiting occupancy of areas with HVAC deficiencies. Partial occupancy with social distancing is a distinctly viable consideration.
Limitations on increasing outside air
Increasing outside air beyond code calculated values requires more energy use and raises utility costs. It can also make the building uncomfortable as the system’s capacity to condition outside air is exceeded. Introducing excessive outside air can raise indoor humidity to a level causing mold growth or, conversely, dry the air to where it produces eye, nose, and throat irritation. It may also increase the introduction of outside air pollutants.
Just open the windows?
While opening windows is often advocated to protect against Covid-19 spread, this may not be effective if site conditions are not favorable. Additionally, careful attention is needed to avoid causing other problems such as creating uncomfortable conditions during hot or cold weather and increasing allergen levels during mild weather. However, it is understood that where there is no HVAC system, opening windows may be the only option for increasing ventilation.
Airflow Patterns
Even where overall ventilation is adequate, the risk of airborne transmission can be higher where room air is not well mixed and airflow patterns create elevated virus concentrations in thebreathing zone. Examples include:
- Wall-mounted fan coil units increase exposure of adjacent occupants (breathing zone is impacted by supply and return air pathways);
- Vent location creates areas with poor air exchange (i.e., spaces without air supply or returns).
An airflow pattern is of major concern where virus is blown between occupants. Although this may occasionally be created by HVAC configuration, the most common cause of this problem is portable devices used to supplement the system (i.e., fans, air purifiers, heaters). Consideration should be given to not allowing occupants to use these.
Non-mechanical ways to compensate for HVAC limitations
In some cases, the most cost-effective way to address HVAC deficiencies is to simply adjust occupancy, for example:
Filtration
If infectious virus actually makes its way through return ducts (i.e., does not inactivate or plate out), filtration can reduce airborne concentrations. Higher efficiency filters have not been shown to reduce COVID-19 transmission and cost more. Study of this important issue has been limited to the measurement of virus deposited on duct surfaces before and after filters. While a MERV-10 pre-filter reduced the amount of deposited SARS-CoV-2 by approximately 70%, downstream, the MERV-15 final filter did not further reduce virus deposits.
Rather than upgrading to higher efficiency filters, a lower-cost way to improve removal of SARS-CoV-2 is to identify and seal by-pass around currently used filters. HVAC filters often do not fit tightly in their frames, allowing air to pass through without particle removal. Eliminating by-pass also improves general indoor air quality.
Will HEPA filter units be effective?
Portable HEPA-filter units remove virus in their immediate vicinity but can also increase occupant exposure where they direct air between occupants, draw their return air through the breathing zone, or blow on surfaces re-suspending virus. Noise generated by these units can also be problematic. Careful design, placement, operation, and maintenance of portable HEPA units is necessary for their effective use. Well-placed HEPA units may be particularly beneficial in areas subject to greater virus exposure, such as bathrooms and elevators.
HVAC Recommendations
Instead of maximizing overall ventilation rates, consider lower-cost changes to HVAC operation to improve air exchange and air mixing include:
Not Recommended
To-date the following measures being advocated for COVID control have not been established in studies to provide additional COVID protection and are generally not cost-effective:
- Increasing ventilation rates beyond ASHRAE minimums;
- Increasing filter efficiency to a minimum of MERV 13;
- Adding humidification;
- Disabling energy recovery wheels;
- UV Disinfection;
- Other forms of air cleaning: bipolar ionization, electrostatic precipitators, hydroxy radical and ozone generators.
How much sanitizing is needed to minimize COVID spread?
To date, insufficient research has been conducted to the extent to which enhanced cleaning is needed to minimize transmission. Although testing has detected SARS-CoV-2 on widely dispersed surfaces, tests for infectious virus have generally been negative. SARS-CoV-2 is easily inactivated by a variety of disinfectants and has even been shown to be controlled by soap.
Only surfaces which may be frequently touched are generally the focus of COVID response. However, occupants also contact other surfaces, and virus settled on any surface can be re-suspended into the air. Enhanced sanitizing should include both sanitizing high touch surfaces as frequently as possible while occupied, and periodically sanitizing other surfaces.
Potential cost-saving measures for minimizing surface transmission
- Purchasing lower-cost sanitizers;
- Omitting initial pre-cleaning step recommended for disinfection if surfaces are visually clean;
- Allowing a shorter dwell time that sanitizer must remain visibly wet on surfaces;
- Reducing application frequency by using a persistent disinfectant;
- Facilitating hands-free contact.
Prioritizing COVID response measures based on available evidence
Priority #1: Enhance personal infection control measures to the extent feasible.Priority #2: Identify high risk conditions and implement appropriate solutions. Such areas can include:- Poor ventilation (i.e., poor low outside air introduced);
- Airflow patterns which concentrate virus (i.e., fans blowing virus between occupants);
- Dense occupancy (i.e., elevators);
- Additional sources of virus (i.e., bathrooms);
- Sensitive occupants (i.e., elderly).
Allocation of resources for COVID control measures in buildings should consider their relative effectiveness. Budgeting for enhanced ventilation, filtration and sanitizing should be balanced against the proven benefits of expanding efforts to increase identification/isolation of infected occupants and staff, masking, social distancing, and handwashing.
Transmission and control of the new variant viruses remain the same and prioritization of building versus occupant control measures does not change. Because the stringency of COVID response measures should consider current community infection rates, rapid spread of a variant would suggest increasing the stringency of response measures.
Reopening School Classrooms, A Cost-Effective Example
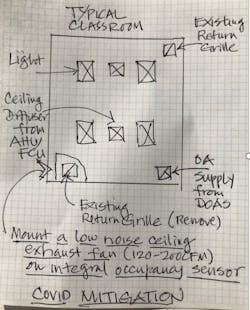
A typical classroom HVAC may have ceiling-mounted fan coil units or VAV supplied by central air handling systems with ducted or plenum returns. In more modern school HVAC design, a DOAS may supply air directly to the classrooms or to the VAV box inlets. While sequences of operations can be modified to improve ventilation, a simple measure using a quiet ceiling exhaust fan located inside the door to increase the air change rate (with the door closed while class is in session). The advantage of this simple scheme is to create an enhanced ventilation exhaust airflow and avoid increasing air mixing. The ceiling diffusers can be best with high ADPI with horizontal airflow pattern. When the door is open, the ceiling exhaust fan will continue to operate by exhausting hallway air that may enter the classroom.
- This sketch from the authors illustrates this measure.
##########
About the authors:
Ed Light is president of Building Dynamics LLC and a Certified Industrial Hygienist (CIH) specializing in indoor air quality (IAQ). Active in the industry for 40 years, he is an AIHA Fellow, member of ASHRAE, author of over 40 peer-reviewed scientific publications and the chair of various national and international committees. Building Dynamics employs mechanical engineers and industrial hygienists following a multi-disciplinary approach to IAQ, HVAC design, and energy management.
Paul Tseng is president of Advanced Building Performance, Inc., which he founded in 2003 to address challenges of wellness in buildings, high performance building systems, deep energy efficiency and system resilience. He is a commissioning specialist with 40 years of experience in HVAC, energy efficiency, and IAQ. A professional engineer, Tseng is also a LEED Fellow, a life member of ASHRAE and the author of many articles for journals such as ASHRAE Journal and HPAC Engineering magazine.
##########
This article presents a summary of information in the Building Dynamics White Paper, Cost-Effective Operations and Maintenance for COVID-19. Included are links to supporting studies and is available, at no cost, from: [email protected].